Your immune system is arguably the most complex and fascinating network within your body, second only to the human brain. It is an intricate, highly coordinated system of cells, tissues, organs, and proteins that work around the clock to defend you against a constant barrage of environmental threats, infectious diseases, viruses, bacteria, and even cellular mutations. When functioning optimally, it acts as a highly trained, internal security force—identifying friend from foe, neutralizing threats, and keeping you vibrant and healthy.
However, the immune system is not invincible. Because it requires a massive amount of metabolic energy and nutritional resources to operate, it can become compromised by various factors, including chronic stress, poor diet, sleep deprivation, underlying medical conditions, or genetic predispositions. When your immune defenses begin to falter, your body will send you warning signs.
Understanding these signs is crucial. Recognizing a weakened immune state early allows you to make proactive, targeted lifestyle changes or seek necessary medical interventions before a minor susceptibility spirals into a severe or chronic health crisis. While everyone occasionally catches a cold or feels run down, there is a distinct difference between standard human illness and a clinically compromised immune system.
In the medical community, recurrent and severe infections are often evaluated using guidelines established by immunological experts. By understanding both the biological mechanisms of immunity and the clinical red flags of immunodeficiency, you can better advocate for your own health.
This comprehensive guide will explore the 10 critical warning signs of a weak immune system, delve deep into the biological reasons behind these symptoms, and provide actionable, science-grounded strategies to help you rebuild your body’s natural defenses.
The Foundation of Immunity: Innate vs. Adaptive
Before diving into the warning signs, it is helpful to understand how your immune system is structured. It is broadly divided into two main branches:
- The Innate Immune System: This is your body’s rapid-response team. It includes physical barriers like your skin and mucous membranes, as well as general-purpose immune cells (like neutrophils and macrophages) that attack any foreign invader they encounter. The innate system is fast but non-specific; it does not remember specific viruses or bacteria.
- The Adaptive Immune System: This is your specialized, targeted defense force. Composed primarily of T-cells and B-cells, the adaptive system takes longer to mobilize but is highly specific. Once it fights off a particular pathogen (like a specific strain of the flu), it creates “memory cells.” If you encounter that exact pathogen again, the adaptive system recognizes it and destroys it before you even feel sick.
When either of these branches is weakened—whether due to secondary lifestyle factors (like stress and malnutrition) or primary genetic disorders (Primary Immunodeficiency)—the clinical warning signs begin to manifest.
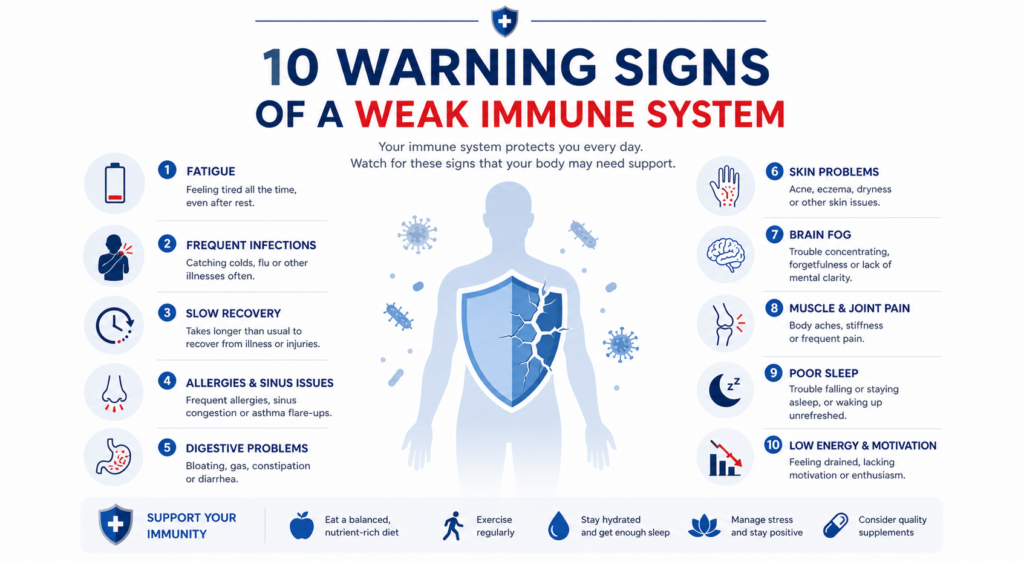
The 10 Warning Signs of a Weak Immune System
The Jeffrey Modell Foundation, a global non-profit organization dedicated to primary immunodeficiency research, developed a widely recognized list of “10 Warning Signs” to help patients and physicians identify underlying immune system defects. While their list is primarily geared toward diagnosing genetic primary immunodeficiencies (PI), these symptoms strongly overlap with acquired, or secondary, immunodeficiencies.
If you consistently experience several of the following ten signs, your immune system may be operating at a significant deficit.
1. Frequent and Recurrent Ear Infections
Ear infections (otitis media) are incredibly common in young children due to the anatomical shape of their developing Eustachian tubes. However, as we grow into adulthood, these tubes become more vertical and efficiently drain fluid, making ear infections relatively rare in healthy adults.
If an adult or older child is experiencing frequent ear infections—specifically, four or more new ear infections within a single year—this is a major red flag. The mucosal lining of the ear, nose, and throat relies heavily on a specific type of antibody called Immunoglobulin A (IgA). IgA is a critical component of your mucosal immunity, acting as a neutralizing barrier that prevents bacteria and viruses from attaching to the delicate tissues of your inner ear.
When your immune system is compromised, or if you suffer from selective IgA deficiency (one of the most common primary immunodeficiencies), the mucosal barriers in your ears become vulnerable. Fluid builds up, opportunistic bacteria like Streptococcus pneumoniae or Haemophilus influenzae take hold, and painful, recurrent infections ensue.
2. Recurrent Pneumonia and Severe Respiratory Infections
Your lungs are constantly exposed to the outside environment with every breath you take. To protect you, the respiratory tract is equipped with a defense mechanism known as the “mucociliary escalator.” Tiny hair-like structures called cilia sweep a sticky layer of mucus upward, trapping dust, viruses, and bacteria so they can be coughed out or swallowed. Furthermore, your lungs contain specialized immune cells called alveolar macrophages, which patrol the air sacs (alveoli) and literally eat foreign pathogens.
A healthy adult might get a mild upper respiratory tract infection (like a common cold) a few times a year, but pneumonia—an infection that inflames the air sacs in one or both lungs—is a serious, deep-seated illness.
Experiencing two or more episodes of pneumonia within a single year is a clear, established warning sign of immune dysfunction. It indicates that your body’s frontline respiratory defenses (like the cilia and mucosal antibodies) and your secondary cellular defenses (like the alveolar macrophages) are failing to stop pathogens before they colonize deep within your lung tissue. This susceptibility is a classic hallmark of both primary immunodeficiencies and secondary immune suppression caused by chronic disease or certain medications.
3. Chronic, Relentless Sinus Infections
Similar to ear infections, sinusitis involves the inflammation and infection of the air-filled cavities behind your cheeks, eyes, and forehead. A standard sinus infection usually resolves within a couple of weeks, either on its own or with a short course of targeted antibiotics.
However, if you suffer from two or more severe sinus infections within a year, or if your sinusitis becomes chronic and resistant to standard treatments, your immune system is likely struggling. Chronic sinusitis in the context of a weak immune system often occurs in the absence of obvious anatomical blockages or severe seasonal allergies.
The mechanism here ties back to the localized mucosal immune system. Your sinuses are protected by Nasal-Associated Lymphoid Tissue (NALT). When B-cells in the NALT fail to produce adequate protective antibodies, or when your innate immune cells become sluggish due to chronic inflammation, normal environmental fungi and bacteria can easily settle into the sinus cavities, form protective biofilms, and cause relentless, painful pressure and infection.
4. Persistent Oral Thrush or Cutaneous Fungal Infections
Thrush is a fungal infection caused by an overgrowth of Candida albicans, a type of yeast. In a healthy body, Candida exists peacefully on your skin, in your digestive tract, and in your mouth. It is kept perfectly in check by your immune system and your body’s natural flora (good bacteria).
However, when your immune system is weakened—particularly if there is a defect in your T-cell function—the Candida yeast can rapidly multiply and cause an active infection. In the mouth, this manifests as oral thrush: thick, creamy white lesions on the tongue, inner cheeks, and roof of the mouth that can bleed when scraped.
While thrush is somewhat common in infants (whose immune systems are still developing) and individuals using inhaled corticosteroids for asthma, persistent or recurrent thrush in an adult is highly abnormal. Similarly, stubborn fungal infections on the skin, such as severe, unyielding ringworm or recurrent yeast infections in skin folds, are significant indicators that your cellular immunity is suppressed and failing to maintain the delicate microscopic balance on your body’s surfaces.
5. Recurrent Deep Skin or Organ Abscesses
Your skin is your largest immune organ, acting as a formidable physical barrier fortified by Skin-Associated Lymphoid Tissue (SALT). When you get a cut or a scratch, innate immune cells called neutrophils rush to the site of the injury to destroy any invading bacteria, such as Staphylococcus aureus.
An abscess is a localized collection of pus—which is essentially a graveyard of dead white blood cells, dead tissue, and bacteria. While anyone can get a minor skin infection from a dirty cut, recurrent, deep-seated abscesses in the skin, or worse, internal organs like the liver or lungs, point to a serious malfunction in your body’s innate immune response.
Conditions like Chronic Granulomatous Disease (CGD) or simple immune exhaustion prevent phagocytes (the cells that “eat” bacteria) from properly destroying the pathogens they ingest. The body tries to wall off the infection by creating an abscess, but because the immune cells cannot finish the job, the abscesses recur deeply and frequently, requiring surgical drainage.
6. Chronic Digestive Issues and Unexplained Diarrhea
You might not immediately associate gut health with immunity, but your digestive tract is the epicenter of your immune defenses. The Gut-associated lymphoid tissue (GALT) makes up approximately 70% of your body’s entire immune system by weight.
The GALT is incredibly complex. It is tasked with a monumental challenge: it must be tolerant of the food you eat and the trillions of beneficial bacteria that make up your microbiome, while remaining highly aggressive toward pathogenic bacteria, viruses, and parasites ingested through your mouth.
When your immune system is weakened, this delicate tolerance is shattered. You may experience chronic diarrhea, profound malabsorption of nutrients, and unexplained weight loss. Without adequate secretory IgA (the primary antibody in the gut) or functional T-cells, opportunistic gut pathogens take over, leading to severe dysbiosis. Chronic diarrhea lasting longer than a few weeks, especially when accompanied by weight loss, is an urgent warning sign that the massive immune network in your gut is compromised.
7. Reliance on Prolonged or Intravenous (IV) Antibiotics
Antibiotics are life-saving medications, but they are designed to work in synergy with your immune system. An antibiotic typically halts the growth of bacteria (bacteriostatic) or kills a portion of them (bactericidal), relying on your body’s white blood cells to come in and clear out the rest of the infection.
If your immune system is weak, the antibiotics have to do all the work on their own. This is often clinically impossible for severe infections. If you find yourself needing two or more months of oral antibiotics with little to no effect, or if minor infections routinely escalate to the point where you require intravenous (IV) antibiotics in a hospital setting, your immune system is waving a massive red flag.
This inability to clear infections even with medical assistance indicates a profound lack of functional immune cells. It also puts you at a high risk for developing antibiotic-resistant superbugs, as the bacteria are exposed to prolonged courses of drugs without being entirely eradicated.
8. Constant, Debilitating Fatigue and Lethargy
Fatigue is a notoriously vague symptom, easily dismissed as a consequence of a busy lifestyle, poor sleep, or aging. However, the profound, unyielding exhaustion associated with a weak or dysregulated immune system is biologically distinct from standard tiredness.
When your immune system is chronically fighting off low-grade infections, dealing with systemic inflammation, or dysregulated, it consumes an enormous amount of metabolic energy (ATP). Furthermore, when immune cells are active, they release chemical messengers called cytokines (like Interleukin-6 and Tumor Necrosis Factor-alpha). These pro-inflammatory cytokines cross the blood-brain barrier and induce what immunologists call “sickness behavior.”
Sickness behavior is an evolutionary adaptation; your brain forces you to feel lethargic, unmotivated, and exhausted so you will lie down, conserve energy, and allow your immune system to utilize your body’s resources to fight the threat. If your immune system is weak and constantly struggling to maintain homeostasis, you will be locked in a state of perpetual “sickness behavior” and chronic fatigue.
9. Immune Dysregulation and Autoimmune Symptoms
It is a common misconception that a “weak” immune system simply means an “underactive” one. In reality, a compromised immune system is often a dysregulated one. When the delicate checks and balances of the immune network fail, the system loses its ability to distinguish between dangerous foreign pathogens and your body’s own healthy tissues.
This breakdown in self-tolerance leads to autoimmunity. A struggling immune system might fail to fight off a common cold, but simultaneously overreact to your own joints, skin, or thyroid gland. Signs of immune dysregulation include the sudden onset of severe eczema, unexplained joint pain (rheumatoid arthritis), thyroid dysfunction (Hashimoto’s or Graves’ disease), or abnormal blood counts such as cytopenias (where the immune system attacks its own red or white blood cells).
If you find yourself constantly sick with infections and suffering from mysterious inflammatory or autoimmune symptoms, it is a glaring sign of a deeply confused and weakened immune network.
10. High Stress Levels and Viral Reactivations
The link between the mind and the immune system is profound, extensively studied in the field of psychoneuroimmunology. Chronic psychological stress acts as a severe immune suppressant. When you are constantly stressed, your adrenal glands pump out high levels of the hormone cortisol, and your sympathetic nervous system remains in “fight or flight” mode.
According to a review of chronic stress and immune dysregulation, persistent cortisol elevation actively inhibits the function of dendritic cells and lymphocytes. It essentially paralyzes your adaptive immune system, specifically suppressing the CD4+ T-cells that coordinate immune responses.
One of the most telling signs of this specific type of immune suppression is viral reactivation. Many of us carry dormant viruses in our bodies, such as the Epstein-Barr Virus (EBV, which causes mononucleosis), Herpes Simplex Virus (cold sores), or Varicella-Zoster (which causes chickenpox and shingles). A strong immune system keeps these viruses permanently locked away in a dormant state. However, when chronic stress dramatically lowers your cellular immunity, these viruses seize the opportunity to reactivate, causing frequent cold sores, unexplained bouts of extreme fatigue, or painful shingles outbreaks. For more information on how systemic stress alters bodily functions, refer to the Centers for Disease Control and Prevention (CDC) guidelines on stress management.
Tables for Quick Reference
To help contextualize these warning signs, the following tables break down the clinical differences between normal illness frequency and immunodeficiency, outline key nutrients required for immune health, and highlight lifestyle factors that dictate immune strength.
Table 1: Normal Illness Frequency vs. Immunodeficiency Warning Signs
Understanding the baseline for normal human illness is important to avoid unnecessary anxiety. Below is a comparison to help you distinguish between an average immune response and a clinically compromised one.
| Health Metric | Normal Immune Function (Adults) | Warning Signs of Weak Immune System / Immunodeficiency |
| Common Colds | 2 to 4 mild colds per year, resolving in 7-10 days. | Chronic, overlapping viral infections; taking weeks to recover from a standard cold. |
| Ear Infections | Rare; perhaps 1 isolated incident every few years. | 4 or more new, distinct ear infections within a single year. |
| Sinus Infections | Occasional, usually triggered by severe allergies or a bad cold; resolves easily. | 2 or more severe sinus infections within a year, often unresponsive to standard care. |
| Pneumonia | Highly uncommon; usually requires a specific severe exposure. | 2 or more confirmed cases of pneumonia within a 1-year timeframe. |
| Antibiotic Efficacy | Standard 7-14 day oral course resolves the bacterial infection. | 2+ months of oral antibiotics with little effect; frequent need for Intravenous (IV) antibiotics. |
| Fungal Infections | Rare; occasional athlete’s foot or easily treatable localized yeast infection. | Persistent oral thrush, recurrent deep skin fungal infections unresponsive to creams. |
Table 2: Key Nutrients and Their Role in the Immune System
A weakened immune system is frequently linked to profound micronutrient deficiencies. Your immune cells require specific vitamins and minerals to metabolize energy, synthesize antibodies, and perform phagocytosis (engulfing pathogens).
| Nutrient | Biological Role in Immunity | Excellent Dietary Sources |
| Vitamin C | Accumulates in phagocytic cells to promote the destruction of microbes; acts as a powerful antioxidant to protect immune cells from self-inflicted oxidative damage. | Citrus fruits, bell peppers, strawberries, broccoli, kiwi, Brussels sprouts. |
| Vitamin D | Enhances the pathogen-fighting effects of monocytes and macrophages; regulates the immune response to prevent autoimmune overreactions. | Sun exposure, fatty fish (salmon, mackerel), fortified dairy, egg yolks, UV-exposed mushrooms. |
| Zinc | Crucial for the normal development and function of cells mediating innate immunity, neutrophils, and NK cells. Zinc deficiency severely impairs T-cell function. | Oysters, beef, pumpkin seeds, lentils, chickpeas, hemp seeds. |
| Selenium | Influences both innate and adaptive immune systems; necessary for the production of glutathione, the body’s master antioxidant. | Brazil nuts, tuna, halibut, sardines, sunflower seeds, chicken. |
| Vitamin A | Maintains the structural and functional integrity of mucosal cells in innate barriers (eyes, lungs, gut); vital for the generation of antibody responses. | Sweet potatoes, carrots, spinach, beef liver, cantaloupe, kale. |
Table 3: Lifestyle Factors: Immune Disruptors vs. Immune Supporters
Your daily habits literally dictate the genetic expression and functional capacity of your immune cells. The choices you make can either suppress your body’s defenses or dramatically enhance them.
| Lifestyle Factor | Immune Disruptor (Causes Weakness) | Immune Supporter (Builds Strength) |
| Sleep Quality | Chronic sleep deprivation (< 6 hours); reduces the production of infection-fighting cytokines and antibodies. | Consistent restorative sleep (7-9 hours); allows the immune system to release essential defensive proteins and consolidate immunological memory. |
| Dietary Patterns | High intake of refined sugars and ultra-processed foods; triggers systemic inflammation and impairs white blood cell phagocytosis for hours after consumption. | A diverse, whole-food diet rich in fiber; feeds the beneficial gut microbiome, which controls 70% of systemic immune responses. |
| Physical Activity | Sedentary lifestyle; leads to poor lymphatic circulation, metabolic stagnation, and higher baseline inflammation. | Regular, moderate exercise (e.g., brisk walking, cycling); promotes the rapid circulation of immune cells and temporary elevation in body temperature to inhibit bacterial growth. |
| Stress Management | Chronic, unmanaged psychological stress; elevates cortisol, continuously suppresses T-lymphocytes, and reactivates dormant viruses. | Active stress reduction (meditation, breathwork, therapy); lowers cortisol, balances the HPA axis, and restores natural killer (NK) cell cytotoxicity. |
Diagnosis: When Should You See a Doctor?
If you recognize yourself in several of the 10 warning signs listed above, it is imperative that you do not attempt to self-diagnose or merely rely on over-the-counter supplements. A truly weakened immune system requires clinical evaluation by a medical professional, often a specialist known as an immunologist.
When you visit a doctor, they will likely start with a thorough medical history, asking about the frequency, severity, and duration of your past infections. From there, specific medical tests can be ordered to objectively measure the strength of your immune defenses. The Mayo Clinic and other leading institutions typically utilize the following diagnostic tools:
- Complete Blood Count (CBC): This is a standard, inexpensive blood test that counts the number of red blood cells, white blood cells, and platelets in your blood. A consistently low white blood cell count (leukopenia), or abnormally low levels of specific immune cells like lymphocytes or neutrophils, is a primary indicator of immune suppression.
- Quantitative Immunoglobulins: This blood test measures the exact levels of the three major types of antibodies in your blood: IgG, IgA, and IgM. Deficiencies in any of these, particularly IgG (which provides long-term protection) or IgA (which protects mucosal surfaces), indicate a primary or acquired immunodeficiency.
- Specific Antibody Responses (Vaccine Titers): A doctor may test your blood to see if your immune system properly responded to past vaccines (like the pneumococcal or tetanus vaccines). If you received a vaccine but your blood shows no protective memory antibodies, your adaptive immune system is failing to create immunological memory.
- Flow Cytometry: For more complex cases, this advanced test analyzes the specific types and subtypes of immune cells in your blood, such as the exact ratio of CD4+ helper T-cells to CD8+ cytotoxic T-cells, which can pinpoint severe cellular deficiencies.
How to Support and Rebuild a Weak Immune System
If clinical testing rules out a genetic primary immunodeficiency, it is highly likely that your immune weakness is secondary—acquired through environmental, dietary, or lifestyle factors. The profoundly encouraging news is that the immune system is highly plastic and responsive. With dedicated effort, you can rebuild your natural defenses.
Here is a scientifically grounded approach to rehabilitating your immune system:
1. Heal and Diversify Your Gut Microbiome
As established, the Gut-Associated Lymphoid Tissue (GALT) commands the vast majority of your immune function. To fix your immune system, you must first fix your gut. This means dramatically increasing your intake of dietary fiber. Fiber acts as a prebiotic, feeding the beneficial bacteria in your colon. These bacteria ferment the fiber into short-chain fatty acids (SCFAs), like butyrate, which directly communicate with and regulate immune cells, reducing systemic inflammation and strengthening the gut barrier. Incorporate a wide variety of plant foods—aiming for 30 different plant types a week—and include fermented foods like kefir, sauerkraut, kimchi, and traditional yogurt.
2. Prioritize Aggressive Rest and Sleep Hygiene
Sleep is not merely a period of inactivity; it is an active, highly structured biological process where the immune system performs its most critical maintenance. During the deep stages of non-REM sleep, your body ramps up the production of protective cytokines and consolidates the “memory” of the T-cells that encountered pathogens during the day. Chronic sleep deprivation acts similarly to a mild immunodeficiency. Ensure your bedroom is completely dark, cool, and free of blue-light emitting screens at least an hour before bed to optimize melatonin production, which itself has potent immune-supporting properties.
3. Modulate Chronic Stress Through Down-Regulation
You cannot completely eliminate stress from modern life, but you can change how your biology responds to it. Because chronic cortisol suppresses T-cell cytotoxicity, you must actively engage your parasympathetic nervous system (the “rest and digest” mode) to counter the sympathetic “fight or flight” drive. Practices such as diaphragmatic breathing, mindfulness meditation, yoga, or even spending time in nature have been clinically shown to lower cortisol and increase the count and activity of Natural Killer (NK) cells.
4. Optimize Micronutrients Safely
While you should aim to get your vitamins and minerals from a diverse, whole-food diet, targeted supplementation can be necessary to correct clinically verified deficiencies. Vitamin D is particularly vital; a large portion of the global population is deficient, and low Vitamin D is directly correlated with an increased risk of respiratory infections and autoimmune diseases. Have your doctor check your 25-hydroxyvitamin D levels, and if they are low, ask for a safe supplementation protocol. Furthermore, ensure adequate intake of Vitamin C, Zinc, and Selenium during times of high physical or emotional stress, as these nutrients are rapidly depleted during active immune responses.
5. Engage in Moderate, Consistent Movement
Exercise is a powerful immune modulator, but the dosage matters. Overtraining or engaging in grueling, extreme endurance events without adequate recovery can actually suppress the immune system temporarily. Conversely, consistent, moderate exercise—like a daily 45-minute brisk walk, swimming, or cycling—is highly beneficial. It promotes the rapid circulation of white blood cells and lymphatic fluid throughout the body, allowing immune cells to detect illnesses earlier. Exercise also helps flush bacteria out of the lungs and airways, reducing the risk of respiratory ailments.
Conclusion
Your immune system is a remarkably resilient and intelligent network, constantly adapting to keep you safe in a microscopic world fraught with danger. However, it requires significant biological support to maintain its vigilance. The 10 warning signs—ranging from persistent ear and sinus infections to chronic fatigue, gut dysfunction, and a relentless reliance on antibiotics—are your body’s desperate plea for help.
Whether these signs point to a hidden primary immunodeficiency requiring specialist intervention, or an acquired weakness due to modern lifestyle stressors, they must not be ignored. By paying close attention to these clinical red flags, seeking proper medical diagnostics, and committing to immune-supporting lifestyle pillars—optimal gut health, restorative sleep, stress mitigation, and dense nutrition—you can empower your body’s internal defense force, reclaim your vitality, and build a lasting foundation of robust health.
References & Scientific Literature
- Jeffrey Modell Foundation (JMF). (n.d.). 10 Warning Signs of Primary Immunodeficiency. Developed by the JMF Medical Advisory Board to increase physician awareness and early diagnosis of primary immunodeficiencies. https://info4pi.org/
- Gut-Associated Lymphoid Tissue (GALT). Wikipedia, The Free Encyclopedia. Overview of the mucosal immune system and its representation of 70% of the body’s immune weight. https://en.wikipedia.org/wiki/Gut-associated_lymphoid_tissue
- Mucosa-Associated Lymphoid Tissue (MALT). Wikipedia, The Free Encyclopedia. Details on the diffuse system of lymphoid tissue in the gastrointestinal tract, nasopharynx, and lungs. https://en.wikipedia.org/wiki/Mucosa-associated_lymphoid_tissue
- Investigating the crosstalk between chronic stress and immune cells: implications for enhanced cancer therapy. Frontiers in Neuroscience (2023). Review paper detailing how chronic stress alters the composition of immune cells, impairs immune responses, and leads to compromised immune effectiveness.
- Gut-associated lymphoid tissue: a microbiota-driven hub of B cell immunity. PMC (2024). Scientific abstract outlining how the diverse gut microbiota maintains GALT in a chronically activated state, necessary for systemic health.
- Evaluation of the 10 Warning Signs in Primary and Secondary Immunodeficient Patients. Frontiers in Immunology (2022). Prospective study validating the JMF scores in differentiating between healthy individuals and those with compromised immunity.
Chronic stress-induced immune dysregulation in cancer.American Journal of Cancer Research (2020). Review illustrating how chronic stress causes a metabolism disorder and prevents the immune system from responding properly to threats.
Emily Carter is a Senior Health Researcher and Supplement Analyst at the Nutrasfit Research Team, based in Austin, Texas. She specializes in evaluating dietary supplements through ingredient analysis, scientific research, and real-world effectiveness.
With a background in nutrition science, Emily focuses on breaking down complex health information into simple, practical insights that readers can trust. Her work is centered on helping individuals make informed decisions and choose supplements that are safe, effective, and aligned with their health goals.