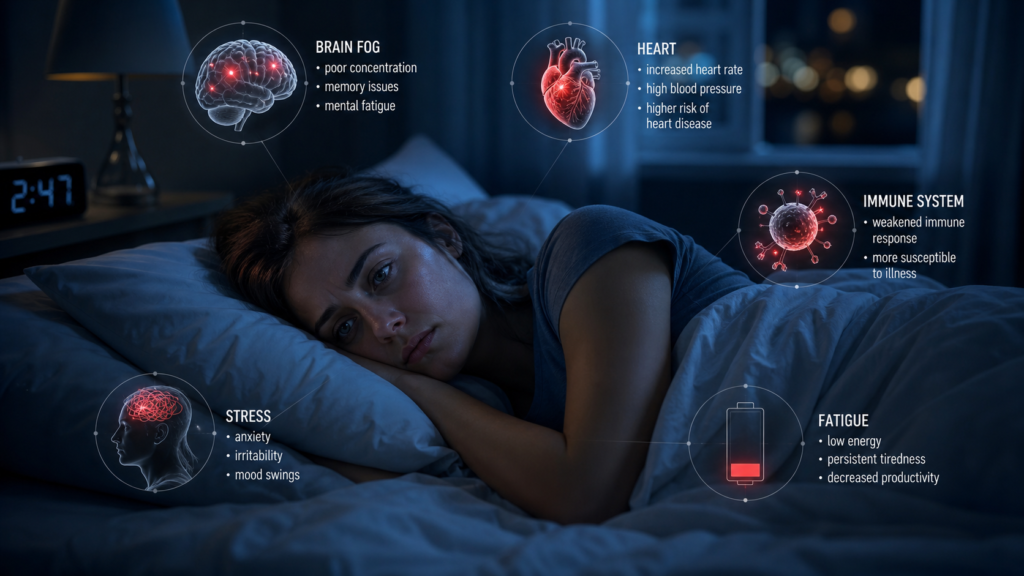
In our hyper-connected, constantly active modern world, sleep is frequently the first casualty of a busy lifestyle. Hustle culture often glorifies sleep deprivation, portraying late nights and early mornings as the ultimate badge of dedication and hard work. However, this societal shift toward chronic sleep restriction is triggering a silent global health crisis.
According to the Centers for Disease Control and Prevention (CDC), adults require an absolute minimum of seven hours of sleep per night for optimal physiological and psychological function. Yet, a staggering one in three adults fails to meet this biological necessity. Sleep is not merely a passive state of rest; it is an incredibly active, highly orchestrated biological process wherein the brain and body engage in critical cellular repair, memory consolidation, toxin removal, and hormonal regulation.
When you consistently shortchange your sleep, you are not just waking up feeling groggy—you are fundamentally altering your body’s biochemistry, impairing your cognitive faculties, and significantly increasing your risk for a multitude of severe, long-term health conditions. From the structural integrity of your brain to the cellular defense mechanisms of your immune system, poor sleep leaves no biological system untouched.
This comprehensive guide delves deeply into the science of sleep deprivation, exploring the top 10 side effects of poor sleep that you simply cannot afford to ignore. We will examine the underlying physiological mechanisms, review findings from clinical research, and outline exactly how chronic sleep debt sabotages your health, well-being, and longevity.
1. Severe Cognitive Impairment and Memory Deficits
One of the most immediate and profound side effects of poor sleep is the deterioration of cognitive function. If you have ever felt “brain fog” after a night of tossing and turning, you have experienced the surface level of this impairment.
The Mechanism of Action
Sleep is divided into multiple stages, including Non-Rapid Eye Movement (NREM) and Rapid Eye Movement (REM) sleep. Deep NREM sleep (specifically N3, or slow-wave sleep) is crucial for declarative memory—the conscious recall of facts and events. During this phase, the brain transfers short-term memories from the hippocampus to the prefrontal cortex, effectively hitting the “save” button on your day’s experiences. REM sleep, on the other hand, is essential for procedural memory (how to do things) and emotional processing.
When sleep is truncated, these memory consolidation processes are abruptly halted. Furthermore, the brain’s glymphatic system—a macroscopic waste clearance system highly active during deep sleep—fails to effectively clear out neurotoxic waste products, including beta-amyloid and tau proteins.
What the Research Says
Studies published by the National Institutes of Health (NIH) have continuously demonstrated that sleep deprivation significantly impairs attention, working memory, and executive function. Chronic accumulation of beta-amyloid plaques, which occur when the glymphatic system is underutilized due to poor sleep, is a primary biomarker and suspected catalyst for neurodegenerative conditions like Alzheimer’s disease. A landmark study from the University of California, Berkeley, found that sleep-deprived individuals experience a massive deficit in their ability to form new memories, acting almost as if the brain’s memory inbox is completely full and unable to receive new files.
2. A Severely Compromised Immune System
Your immune system and your sleep cycles are inextricably linked. Sleep deprivation acts as an immunosuppressant, drastically reducing your body’s ability to fend off invading pathogens, viruses, and bacterial infections.
The Mechanism of Action
During high-quality sleep, your immune system releases specialized proteins called cytokines. Certain cytokines are specifically designed to promote sleep, while others are ramped up during times of infection, inflammation, or acute stress. Sleep deprivation fundamentally decreases the production of these protective, infection-fighting cytokines. Additionally, chronic sleep loss reduces the proliferation and effectiveness of vital immune cells, including T-cells and Natural Killer (NK) cells, which act as the body’s frontline soldiers against viral infections and malignant tumor cells.
What the Research Says
Research featured in the Journal of Experimental Medicine highlights that sleep actually enhances the ability of T-cells to adhere to and destroy cells infected by viruses. In stark contrast, individuals who consistently sleep fewer than six hours per night are more than four times as likely to catch the common cold compared to those who sleep seven or more hours, according to studies monitored by the Mayo Clinic. Furthermore, inadequate sleep severely blunts the body’s immunological response to vaccines. A seminal study investigating the efficacy of the influenza vaccine showed that sleep-deprived subjects produced significantly fewer antibodies than their well-rested counterparts, leaving them critically unprotected despite receiving the vaccination.
3. Increased Risk of Cardiovascular Disease and Hypertension
The heart is arguably the hardest-working organ in the human body, beating around 100,000 times a day. Sleep provides a rare and essential window of reduced cardiovascular demand, allowing the heart to rest and repair. Denying the body this recovery period leads to severe cardiovascular strain.
The Mechanism of Action
In healthy, restful sleep, a phenomenon known as “nocturnal dipping” occurs. Blood pressure naturally drops by about 10% to 20%, and the resting heart rate slows down significantly. This easing of the cardiovascular workload is vital for the long-term maintenance of the heart and blood vessels. When sleep is interrupted or too short, the body remains trapped in a state of high sympathetic nervous system arousal (the “fight or flight” response). This prolonged arousal leads to a sustained overproduction of stress hormones like cortisol and adrenaline, which keep blood pressure elevated throughout the night and into the following day.
What the Research Says
The American Heart Association (AHA) officially recognizes sleep as a critical pillar of cardiovascular health. Research indicates that chronic short sleepers (those getting less than 6 hours per night) have a profoundly higher risk of developing hypertension (high blood pressure). Over time, this constant mechanical stress on the arterial walls causes micro-tears, leading to atherosclerosis (the buildup of plaque). Consequently, epidemiological studies have repeatedly shown that poor sleep is independently associated with a dramatically increased risk of fatal heart attacks, arrhythmias, and strokes.
4. Metabolic Dysregulation, Weight Gain, and Obesity

If you have ever found yourself craving sugary, high-carbohydrate, or greasy foods after a poor night of sleep, you are not simply experiencing a lack of willpower; you are fighting a massive physiological shift in your hormonal landscape. Poor sleep is one of the strongest risk factors for obesity.
The Mechanism of Action
Sleep heavily dictates the delicate balance of two highly influential appetite-regulating hormones: ghrelin and leptin. Ghrelin is the hormone that signals hunger to the brain, while leptin is the hormone that signals satiety (fullness). When you are sleep-deprived, ghrelin levels spike dramatically, and leptin levels plummet. This creates a biological imperative to eat, even if you do not physically require the calories.
Furthermore, sleep deprivation alters the brain’s endocannabinoid system—the same system affected by marijuana—which amplifies the perceived reward and pleasure derived from eating highly palatable, calorie-dense foods. Additionally, being awake longer naturally provides a wider window of time to eat, often leading to late-night snacking when metabolic efficiency is at its lowest.
What the Research Says
Endocrinology studies from institutions like the University of Chicago have demonstrated that sleep-deprived individuals consume an average of 300 to 500 extra calories per day compared to when they are well-rested. Long-term observational data published in the American Journal of Clinical Nutrition supports the notion that chronic sleep restriction is inextricably linked to higher Body Mass Index (BMI) and expanded waist circumferences. By sabotaging your appetite control and driving intense cravings for junk food, poor sleep makes weight management an uphill, almost impossible battle.
5. Severe Mental Health Deterioration: Anxiety and Depression
The bidirectional relationship between sleep and mental health is profound. While psychiatric disorders can cause sleep disturbances, poor sleep is equally capable of instigating and drastically worsening mental health conditions, particularly anxiety and major depressive disorder.
The Mechanism of Action
During REM sleep, the brain actively processes the emotional experiences of the day in a neurochemical environment devoid of noradrenaline (a stress-inducing neurotransmitter). This acts as a form of overnight emotional therapy, allowing us to wake up feeling emotionally balanced and rational.
When sleep is cut short, the brain’s emotional center, the amygdala, becomes hyperactive. Functional MRI scans have revealed that sleep-deprived brains exhibit up to a 60% increase in amygdala reactivity to negative stimuli. Simultaneously, the neural connections between the amygdala and the medial prefrontal cortex—the logical, rational part of the brain that normally keeps emotional responses in check—are physically severed. This leaves the sleep-deprived individual emotionally volatile, irritable, and highly vulnerable to anxiety.
What the Research Says
According to clinical research from the National Alliance on Mental Illness (NAMI), individuals suffering from insomnia have a tenfold higher risk of developing clinical depression and a seventeen-fold increased risk of severe anxiety disorders compared to those who sleep normally. Chronic sleep loss deeply alters mood regulation, dampens enthusiasm, lowers the threshold for frustration, and, in severe cases, is strongly correlated with an increased risk of suicidal ideation.
6. Endocrine Disruption and Lowered Libido
Sleep is the ultimate master regulator of the endocrine (hormonal) system. When you do not get adequate rest, virtually every hormone in your body is thrown out of its natural circadian rhythm, resulting in systemic physiological disruptions, including a noticeable collapse in sexual health and vitality.
The Mechanism of Action
The majority of testosterone production in both men and women occurs during the deep phases of sleep. When sleep is continually restricted or fragmented—such as in cases of untreated obstructive sleep apnea—testosterone levels plummet. At the same time, the body compensates for the lack of sleep by pumping out high volumes of cortisol, the primary stress hormone. Cortisol and reproductive hormones have an antagonistic relationship; when cortisol is chronically high, reproductive hormones are suppressed, leading to a drastically reduced sex drive.
What the Research Says
The Journal of the American Medical Association (JAMA) published a notable study showing that young, healthy men who restricted their sleep to just five hours a night for a single week experienced a massive drop in testosterone levels, equivalent to aging 10 to 15 years. For women, sleep deprivation leads to similar hormonal chaos, impacting not just libido but also the regularity of the menstrual cycle and overall fertility. The Sleep Foundation notes that exhaustion, tension, and the hormonal imbalances caused by sleep deprivation act as a potent anti-aphrodisiac, severely impacting intimacy and relationship satisfaction.
7. Impaired Glucose Tolerance and Increased Risk of Type 2 Diabetes
Sleep deprivation fundamentally alters the way your body processes food at a cellular level, particularly how it handles sugars and carbohydrates. Chronic poor sleep is recognized by medical professionals as a direct physiological pathway to prediabetes and Type 2 diabetes.
The Mechanism of Action
Deep, restorative slow-wave sleep plays a pivotal role in regulating blood glucose levels. During healthy sleep, insulin—the hormone responsible for ushering glucose from the bloodstream into the cells for energy—functions highly efficiently.
However, when you are sleep-deprived, the cells in your body become “insulin resistant.” This means the cells stop responding properly to insulin’s signals. As a result, glucose remains circulating in the blood. To compensate for this elevated blood sugar, the pancreas is forced into overdrive, pumping out even more insulin. Over time, this constant strain can exhaust the pancreatic beta cells, eventually leading to full-blown Type 2 diabetes. The persistent elevation of cortisol due to sleep loss further exacerbates the problem, as cortisol naturally prompts the liver to release stored glucose into the bloodstream.
What the Research Says
Clinical experiments have shown alarming results. Healthy, non-diabetic adults who were restricted to just four hours of sleep a night for a mere six consecutive days experienced a staggering 40% decrease in their ability to clear glucose from their bloodstream. Their metabolic state closely resembled that of an elderly, pre-diabetic individual. The CDC and the American Diabetes Association (ADA) clearly emphasize that improving sleep duration and quality is absolutely essential for glycemic control and metabolic health.
8. Accelerated Cellular Aging and Premature Skin Degradation
The concept of “beauty sleep” is not a myth; it is an undeniable biological reality rooted in cellular regeneration. Chronic sleep deprivation aggressively accelerates the physical signs of aging, particularly impacting the health, elasticity, and appearance of the skin.
The Mechanism of Action
The skin is the body’s largest organ, and it undergoes immense repair during the night. Deep sleep is characterized by a surge in the secretion of Human Growth Hormone (HGH), a vital polypeptide that facilitates tissue repair, muscle growth, and cellular regeneration throughout the body. HGH is essential for maintaining the structural integrity of the skin matrix.
Conversely, poor sleep causes a sustained elevation in cortisol. Cortisol is highly destructive to collagen—the primary structural protein that keeps the skin firm, elastic, and youthful. Furthermore, sleep deprivation impairs the skin’s barrier function, leading to increased transepidermal water loss. This leaves the skin dehydrated, prone to irritation, and incapable of defending itself against environmental stressors like UV radiation and pollution.
What the Research Says
Studies published in clinical dermatology journals reveal that poor sleepers exhibit significantly more signs of intrinsic skin aging, including fine lines, uneven pigmentation, and reduced skin elasticity. A widely cited study evaluated by the University Hospitals Case Medical Center found that women who consistently slept poorly had double the visible signs of aging compared to well-rested women. Moreover, their skin recovered much slower from environmental stressors like sunburns, highlighting a deeply compromised regenerative capacity.
9. Severe Motor Impairment and Increased Risk of Accidents
Perhaps one of the most immediate, life-threatening side effects of poor sleep is the catastrophic impact it has on reaction times, spatial awareness, and psychomotor vigilance. Being awake for an extended period impairs your brain to the same degree as being legally intoxicated.
The Mechanism of Action
When the brain is desperately starved for sleep, it begins to force itself into micro-sleeps. Microsleeps are brief, involuntary episodes of sleep that can last anywhere from a fraction of a second up to 30 seconds. During a microsleep, the brain essentially shuts down, rendering the individual completely blind and unresponsive to their environment, even if their eyes remain physically open.
Furthermore, sleep deprivation severely degrades the communication between sensory input (what you see or hear) and motor output (your physical reaction). This means that even if you manage to stay awake, your ability to react swiftly to sudden hazards is drastically slowed down.
What the Research Says
The National Highway Traffic Safety Administration (NHTSA) estimates that drowsy driving is responsible for tens of thousands of crashes, injuries, and fatalities every single year. Shockingly, scientific studies have equated the cognitive impairment of staying awake for 18 hours straight to having a Blood Alcohol Concentration (BAC) of 0.05%. Staying awake for 24 hours pushes that impairment to a BAC of 0.10%—well above the legal driving limit in most jurisdictions. Operating a vehicle or heavy machinery while sleep-deprived is not just irresponsible; it is highly dangerous and statistically comparable to drunk driving.
10. Systemic, Chronic Inflammation
While acute inflammation is a necessary and healthy response to injury or acute infection, chronic systemic inflammation is a silent killer. It is recognized as a root cause or accelerating factor for almost every major age-related disease, and poor sleep is a primary driver of this inflammatory state.
The Mechanism of Action
Sleep acts as a systemic “cooling down” period for the body’s inflammatory markers. When sleep is chronically restricted or highly fragmented, the sympathetic nervous system remains overactive, and the body interprets this lack of rest as a persistent state of physical stress or danger. In response, the body continuously pumps out pro-inflammatory markers, including C-reactive protein (CRP) and Interleukin-6 (IL-6).
This state of low-grade, chronic inflammation circulates throughout the entire body, silently attacking healthy tissues, damaging blood vessels, and accelerating cellular wear and tear.
What the Research Says
Extensive epidemiological studies published in reputable medical journals demonstrate a clear, dose-dependent relationship between sleep duration and inflammatory markers. Individuals who consistently sleep less than six hours per night exhibit chronically elevated levels of CRP and IL-6. This rampant inflammation is a common denominator linking poor sleep to autoimmune flare-ups, chronic pain conditions, rheumatoid arthritis, gastrointestinal disorders like inflammatory bowel disease (IBD), and certain types of cancer. By actively prioritizing sleep, you are implementing a powerful, natural anti-inflammatory intervention.
Strategic Interventions: How to Reclaim Your Sleep and Your Health
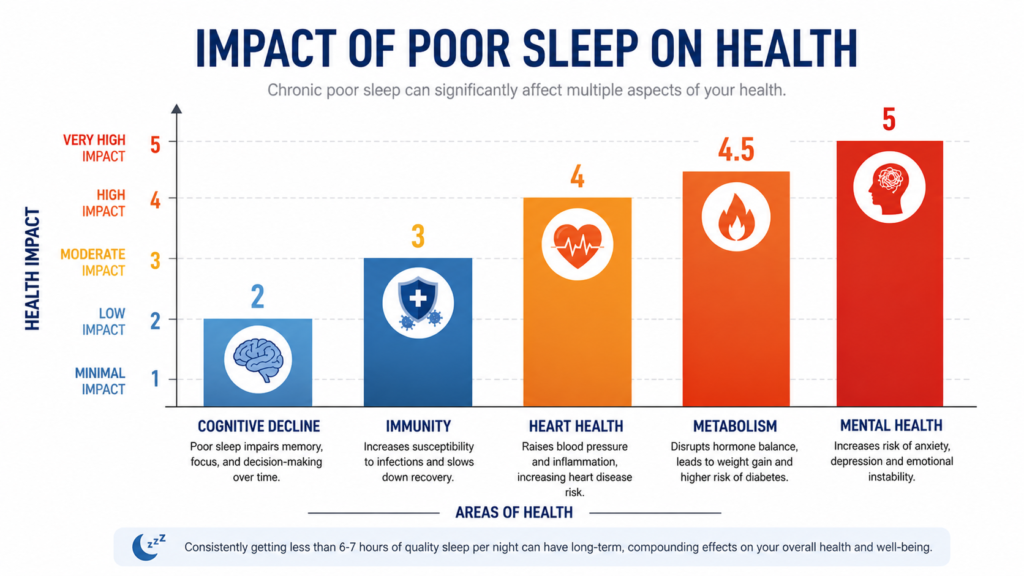
Understanding the devastating side effects of sleep deprivation is only the first step. The critical next phase is implementing actionable, science-backed strategies to optimize your sleep architecture and restore your biological equilibrium. Reversing sleep debt requires a dedicated approach to “sleep hygiene.”
1. Optimize Your Circadian Rhythm
Your body operates on an internal 24-hour clock known as the circadian rhythm. To anchor this rhythm, consistency is paramount.
- Set a Strict Schedule: Go to bed and wake up at the exact same time every day, including weekends. This predictability allows your brain to optimize the release of melatonin (the sleep hormone) in the evening and cortisol (for wakefulness) in the morning.
- Morning Sunlight Exposure: Step outside into natural sunlight for 10 to 15 minutes within an hour of waking. This halts the production of residual melatonin and sets a biological timer for sleep later that night.
2. Curate a Sleep-Inducing Environment
Your bedroom should be a sanctuary optimized strictly for sleep and intimacy.
- Temperature Control: The human body needs to drop its core temperature by about 2 to 3 degrees Fahrenheit to initiate and sustain deep sleep. Keep your bedroom cool, ideally between 60°F and 67°F (15°C to 19°C).
- Total Darkness: Light is the most powerful inhibitor of melatonin. Invest in high-quality blackout curtains or wear a comfortable eye mask. Even tiny ambient lights from electronics can disrupt your sleep architecture.
- Minimize Noise: Use earplugs or a white noise machine to block out unpredictable environmental sounds that can pull you out of deep sleep stages.
3. Master Light and Technology Exposure
In the modern era, artificial light at night is the greatest enemy of healthy sleep.
- Beware of Blue Light: The blue light emitted by smartphones, tablets, computers, and LED lights strongly suppresses melatonin production by tricking your brain into thinking it is still daytime.
- Implement a Digital Sunset: Enforce a strict “no-screens” policy at least 60 to 90 minutes before bed. Swap scrolling on your phone for relaxing activities like reading a physical book, gentle stretching, or taking a warm bath (which paradoxically helps lower your core body temperature afterward).
4. Manage Nutritional and Chemical Intakes
What you put into your body directly influences how well you sleep.
- Caffeine Curfew: Caffeine is a powerful stimulant with a half-life of roughly 5 to 7 hours, and a quarter-life of up to 12 hours. This means that a coffee consumed at 3:00 PM can still be keeping your brain wired at midnight. Impose a strict caffeine curfew by 12:00 PM or 2:00 PM at the latest.
- Avoid Alcohol Before Bed: While alcohol is a sedative that might help you lose consciousness faster, it is absolutely destructive to sleep quality. It actively blocks REM sleep and heavily fragments your rest, leading to frequent micro-awakenings throughout the night.
- Mind Your Meals: Avoid large, heavy, or highly spicy meals within three hours of bedtime to prevent indigestion and acid reflux, which can ruin sleep continuity.
5. Seek Professional Medical Guidance When Necessary
If you have optimized your sleep hygiene, maintained a consistent schedule, and still struggle with chronic insomnia, excessive daytime sleepiness, loud snoring, or waking up gasping for air, you must consult a healthcare professional. You may be suffering from an underlying clinical sleep disorder, such as Obstructive Sleep Apnea (OSA) or Restless Legs Syndrome (RLS).
For severe insomnia, physicians often recommend Cognitive Behavioral Therapy for Insomnia (CBT-I). CBT-I is a structured, highly effective, evidence-based program that targets the underlying thoughts, anxieties, and behaviors that are sabotaging your sleep, proving far more effective long-term than prescription sleep medications.
Conclusion: The Biological Non-Negotiable
Sleep is not a luxury, an indulgence, or a state of unproductive idleness. It is a fundamental biological imperative—a highly active, non-negotiable pillar of health that is intrinsically tied to every physiological system in the human body. The glorification of sleep deprivation must end, replaced by a deep cultural respect for the profound healing and regenerative power of rest.
From destroying cognitive faculties and paralyzing the immune system to accelerating aging and inviting severe chronic diseases like diabetes and heart failure, the side effects of poor sleep are vast, insidious, and life-altering. By consistently achieving seven to nine hours of high-quality sleep per night, you are not just preventing disease; you are actively investing in your mental clarity, emotional resilience, physical vitality, and overall longevity. It is time to treat your sleep with the absolute reverence it deserves.
Authoritative References and Further Reading
For those looking to explore the science of sleep and its profound impact on human health more deeply, the following resources, institutions, and databases provide authoritative, peer-reviewed information:
- Centers for Disease Control and Prevention (CDC) – Sleep and Sleep Disorders: A comprehensive overview of public health guidelines, sleep hygiene tips, and statistical data regarding the sleep epidemic. CDC Sleep Guidelines
- National Institutes of Health (NIH) – National Heart, Lung, and Blood Institute (NHLBI): Detailed, research-backed articles explaining the physiological importance of sleep and the mechanisms of various sleep disorders. NIH Sleep Science
- The Sleep Foundation: An independent, trusted resource offering deep dives into sleep science, mattress reviews, and actionable advice for overcoming insomnia. SleepFoundation.org
- American Heart Association (AHA): Resources detailing the critical, undeniable link between sleep quality, hypertension, and long-term cardiovascular health. AHA Healthy Sleep
- American Diabetes Association (ADA): Clinical insights into how sleep deprivation sabotages glucose metabolism and increases insulin resistance. Diabetes.org
- National Highway Traffic Safety Administration (NHTSA): Eye-opening statistics and safety campaigns regarding the extreme dangers of drowsy driving and micro-sleeps. NHTSA Drowsy Driving
- Wikipedia – The Glymphatic System: A detailed scientific breakdown of how the brain clears neurotoxic waste during deep, slow-wave sleep. Glymphatic System Overview
National Alliance on Mental Illness (NAMI): Extensive literature on the bidirectional relationship between sleep deprivation and severe psychiatric disorders, including anxiety and depression. NAMI Sleep and Mental Health
Emily Carter is a Senior Health Researcher and Supplement Analyst at the Nutrasfit Research Team, based in Austin, Texas. She specializes in evaluating dietary supplements through ingredient analysis, scientific research, and real-world effectiveness.
With a background in nutrition science, Emily focuses on breaking down complex health information into simple, practical insights that readers can trust. Her work is centered on helping individuals make informed decisions and choose supplements that are safe, effective, and aligned with their health goals.