
Waking up after a full night’s sleep only to feel as though you have run a marathon in your dreams is a deeply frustrating and disheartening experience. You did everything right—you went to bed early, you turned off your screens, and you stayed in bed for eight hours—yet your body feels heavy, your limbs feel weak, and your mind is clouded with brain fog. If you are experiencing this, you are not alone, and your feelings are entirely valid.
While society often equates tiredness with a simple lack of sleep, the reality of human physiology is far more complex. Rest and sleep are not always synonymous with recovery. When you feel weak despite adequate rest, your body is sending you a clear signal that something within your internal systems—whether cellular, metabolic, hormonal, or psychological—is out of balance.
This comprehensive guide delves deep into the biological, environmental, and psychological reasons why your body feels weak even after rest. By understanding the underlying mechanisms, you can begin to pinpoint the root cause of your exhaustion and take actionable steps toward true restoration.
1. Defining the Disconnect: Fatigue vs. Weakness
Before exploring the causes, it is crucial to understand the medical distinction between fatigue and weakness, as they often overlap but represent different physiological states.
- Fatigue: A subjective feeling of tiredness, exhaustion, or lack of energy. It is an overall systemic sensation that makes it difficult to initiate or sustain physical or mental activities.
- Weakness (Asthenia): A lack of physical or muscle strength. It is the feeling that extra effort is required to move your arms, legs, or body. True clinical weakness can be measured (e.g., reduced grip strength), whereas perceived weakness is the sensation that your muscles are failing, even if they can still perform tasks.
When you feel “weak” after resting, you are likely experiencing a combination of profound systemic fatigue and perceived muscle weakness. This indicates a failure in how your body generates, conserves, or utilizes energy.
2. The Cellular Level: How Your Body Creates Energy
To understand why you lack energy, we must first look at how your body produces it. The human body does not run directly on the food you eat; it runs on a molecule called Adenosine Triphosphate (ATP).
The Role of Mitochondria
Mitochondria are often referred to as the “powerhouses” of the cells. Found in almost every cell in your body, these tiny organelles take the glucose from your food and the oxygen from your blood and convert them into ATP through a complex process known as cellular respiration.
If your mitochondria are malfunctioning, or if they lack the necessary raw materials (like oxygen, vitamins, or minerals) to produce ATP efficiently, your cells will literally be starved of energy. This cellular starvation translates to systemic fatigue and muscle weakness. Even if you sleep for twelve hours, if your cells cannot produce ATP, you will wake up feeling exhausted.
3. Sleep Architecture: Quantity vs. Quality
One of the most common reasons people feel weak after resting is a fundamental misunderstanding of sleep. Time spent unconscious does not automatically equal time spent recovering. Sleep is divided into distinct cycles, each lasting roughly 90 to 110 minutes, and each cycle contains different stages.
The Stages of Sleep
- Stage 1 (Light Sleep): The transition between wakefulness and sleep.
- Stage 2 (Light Sleep): Heart rate slows, and body temperature drops.
- Stage 3 (Deep Sleep / Slow-Wave Sleep): This is the most crucial stage for physical recovery. During deep sleep, your body repairs tissues, builds bone and muscle, and strengthens the immune system. Blood flow to the muscles increases.
- REM (Rapid Eye Movement) Sleep: Crucial for cognitive function, memory consolidation, and emotional regulation.
The Problem of Fragmented Sleep
If your sleep architecture is constantly interrupted—even if you do not fully wake up—you may never spend enough time in Stage 3 Deep Sleep or REM sleep. You can be in bed for nine hours but only get a few minutes of restorative deep sleep. This is known as fragmented sleep, and it leaves your body physically un-repaired and profoundly weak.
4. Hidden Sleep Disorders
Many people suffer from sleep disorders for years without realizing it, attributing their daily weakness to aging or stress.
Obstructive Sleep Apnea (OSA)
Obstructive Sleep Apnea is a serious condition where the muscles in the back of the throat fail to keep the airway open, despite efforts to breathe. This causes breathing to repeatedly stop and start during sleep.
Every time your airway collapses, your blood oxygen levels plummet. Your brain detects this danger and briefly wakes you up to reopen the airway. This can happen dozens or even hundreds of times a night. Because you are constantly being jolted out of deep sleep, your body is effectively fighting for its life all night instead of resting. For more information, you can read the comprehensive overview of Sleep Apnea on the Mayo Clinic website.
Restless Legs Syndrome (RLS) and Periodic Limb Movement Disorder (PLMD)
RLS causes an uncontrollable urge to move your legs, usually due to an uncomfortable sensation. PLMD involves involuntary cramping or jerking of the legs during sleep. Both conditions severely disrupt the sleep cycle, leading to extreme morning exhaustion.
Table 1: Common Sleep Disorders and Their Hidden Symptoms
| Sleep Disorder | Primary Mechanism | Symptoms Beyond Fatigue |
| Obstructive Sleep Apnea | Airway blockage causing oxygen desaturation. | Loud snoring, waking up gasping, morning headaches, dry mouth. |
| Insomnia | Inability to initiate or maintain sleep. | Anxiety around bedtime, waking up too early, cognitive impairment. |
| Narcolepsy | Neurological inability to regulate sleep-wake cycles. | Sudden loss of muscle tone (cataplexy), sleep paralysis, hallucinations. |
| Restless Legs Syndrome | Neurological sensory disorder, often linked to dopamine or iron. | “Crawling” sensation in legs, worse in the evening or when lying down. |
5. Nutritional Deficiencies: Running on Empty
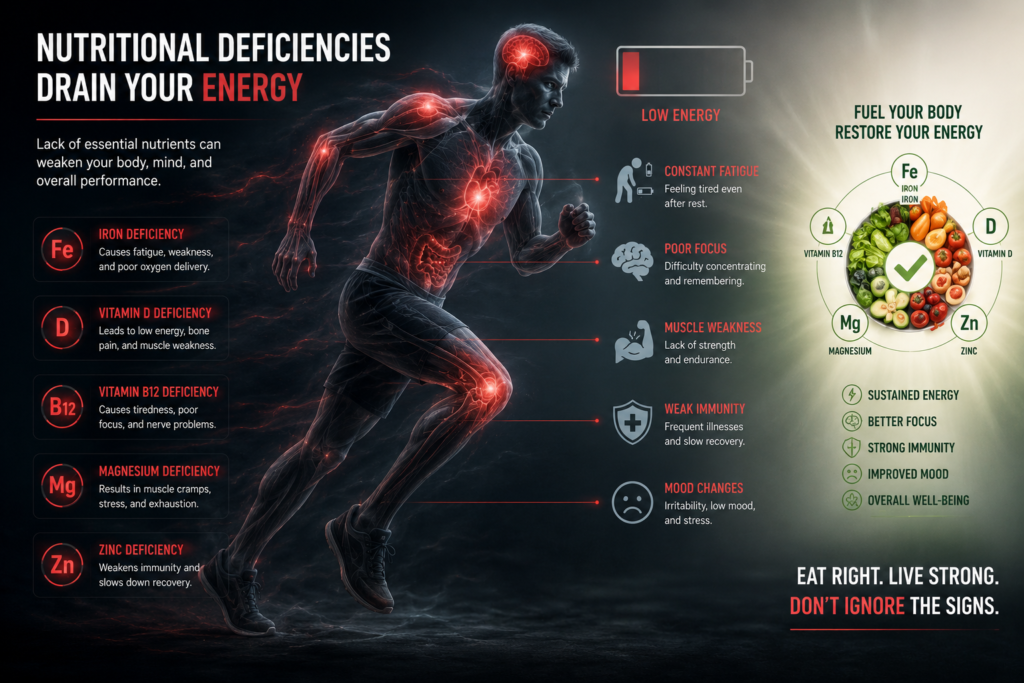
Even if your sleep is perfect, your body cannot function without the proper building blocks. Nutritional deficiencies are among the most common, yet easily correctable, causes of chronic weakness.
Iron Deficiency Anemia
Iron is a vital component of hemoglobin, the protein in red blood cells that carries oxygen from your lungs to the rest of your body. If you lack iron, your body cannot produce enough healthy red blood cells. Without sufficient oxygen reaching your tissues and muscles, ATP production grinds to a halt, resulting in profound weakness, shortness of breath, and pale skin.
Vitamin B12 Deficiency
Vitamin B12 is essential for nerve function and the production of DNA and red blood cells. A deficiency can lead to a specific type of anemia (megaloblastic anemia) where red blood cells are abnormally large and inefficient. Furthermore, B12 is crucial for maintaining the myelin sheath (the protective coating around nerves). A lack of B12 can cause neurological symptoms, including muscle weakness, tingling in the extremities, and cognitive decline. The National Institutes of Health (NIH) provides extensive data on Vitamin B12.
Vitamin D Deficiency
Often called the “sunshine vitamin,” Vitamin D functions more like a hormone in the body. It is critical for bone health, immune function, and muscle function. Severe Vitamin D deficiency is strongly linked to skeletal muscle weakness, deep bone pain, and a pervasive sense of physical heaviness.
Magnesium Deficiency
Magnesium is involved in over 300 biochemical reactions in the body, including muscle and nerve function, blood glucose control, and energy production. Low magnesium levels can lead to muscle cramps, spasms, and a general feeling of physical exhaustion.
Table 2: Key Nutrients for Energy and Their Sources
| Nutrient | Role in Energy Production | Common Food Sources |
| Iron | Oxygen transport via hemoglobin. | Red meat, lentils, spinach, fortified cereals. |
| Vitamin B12 | Nerve health, red blood cell formation. | Meat, fish, dairy, eggs, fortified nutritional yeast. |
| Vitamin D | Muscle function, bone health. | Sun exposure, fatty fish, egg yolks, fortified milk. |
| Magnesium | ATP production, muscle relaxation. | Almonds, spinach, black beans, pumpkin seeds. |
6. Endocrine and Metabolic Disruptors
Your endocrine system is a network of glands that produce hormones regulating metabolism, growth, tissue function, and sleep. When this system is dysregulated, your energy levels will plummet regardless of how much you rest.
Hypothyroidism (Underactive Thyroid)
The thyroid gland, located in your neck, is the master controller of your metabolism. It produces hormones (T3 and T4) that tell your cells how fast to use energy. In hypothyroidism, the gland does not produce enough of these hormones. As a result, your entire metabolism slows down. Symptoms include profound weakness, unexplained weight gain, feeling cold constantly, and sluggish digestion. No amount of sleep can cure the fatigue caused by an underactive thyroid; it requires medical intervention and hormone replacement.
Blood Sugar Dysregulation and Insulin Resistance
If your diet is high in refined carbohydrates and sugars, you may experience rapid spikes and crashes in your blood glucose levels. A “sugar crash” leaves you feeling weak and shaky. Over time, chronic high blood sugar can lead to insulin resistance, a precursor to Type 2 Diabetes. When your cells become resistant to insulin, they cannot effectively absorb glucose from your bloodstream. Your cells are essentially starving for energy while swimming in a sea of unused sugar, leading to chronic fatigue.
Adrenal Fatigue vs. HPA Axis Dysregulation
While the term “adrenal fatigue” is popular in alternative medicine, endocrinologists generally recognize this phenomenon as Hypothalamic-Pituitary-Adrenal (HPA) axis dysregulation. Chronic stress keeps your cortisol (the stress hormone) levels constantly elevated. Over time, this chronic activation burns out the feedback loops between your brain and adrenal glands. You may end up with a flattened cortisol curve, meaning your body struggles to produce the energy needed to wake up in the morning, leaving you feeling profoundly exhausted upon waking.
7. Chronic, Immune, and Post-Viral Conditions
Sometimes, the body’s own defense mechanisms become the source of exhaustion.
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)
ME/CFS is a complex, deeply debilitating neurological disease. The hallmark symptom is Post-Exertional Malaise (PEM), where minor physical or mental exertion results in a severe crash in energy that can last for days or weeks. For someone with ME/CFS, rest does not alleviate the fatigue. The exact cause is unknown, but it is often triggered by a viral infection and involves systemic dysfunction of the immune, neurological, and energy metabolism systems. You can read more about the diagnostic criteria and ongoing research on Wikipedia’s ME/CFS page.
Fibromyalgia
Fibromyalgia is characterized by widespread musculoskeletal pain accompanied by fatigue, sleep, memory, and mood issues. Researchers believe that fibromyalgia amplifies painful sensations by affecting the way your brain and spinal cord process pain and nonpain signals. The constant barrage of pain signals severely disrupts deep sleep, leading to unrefreshing sleep and profound morning weakness.
Autoimmune Diseases
Conditions like Rheumatoid Arthritis, Lupus, and Multiple Sclerosis involve the immune system mistakenly attacking healthy tissues. The constant state of systemic inflammation requires a massive amount of the body’s energy. Your immune system is effectively fighting a never-ending war inside your body, which diverts energy away from your muscles and brain, leaving you exhausted.
Post-Viral Fatigue (Including Long COVID)
It is very common to feel weak for weeks after a severe viral infection (like the flu, Epstein-Barr virus, or COVID-19). The body requires immense energy to clear the virus and repair the damage. In conditions like Long COVID, this fatigue can persist for months or years, likely due to lingering inflammation, viral persistence, or damage to the autonomic nervous system.
8. The Mind-Body Connection: Psychological Factors
The brain consumes about 20% of the body’s energy. Psychological burdens are not just “in your head”; they have a tangible, heavy physical toll on your body.
Depression
Depression is deeply physical. It alters the balance of neurotransmitters like serotonin, dopamine, and norepinephrine, which regulate energy, motivation, and sleep. People suffering from depression often experience hypersomnia (sleeping too much) but never feel rested. The physical sensation of depression is often described as moving through molasses or wearing a lead suit. For more details on the systemic symptoms of depression, the Centers for Disease Control and Prevention (CDC) offers a comprehensive guide.
Anxiety and Chronic Stress
Living with chronic anxiety means your body is stuck in a “fight or flight” state. Your sympathetic nervous system is highly active, your heart rate is elevated, and your muscles are constantly tense. Even when you lie down to rest, your brain is scanning for threats. This chronic state of hyperarousal prevents restorative deep sleep and depletes your energy reserves.
Burnout
Burnout is an occupational phenomenon resulting from chronic workplace stress that has not been successfully managed. It is characterized by feelings of energy depletion, increased mental distance from one’s job, and reduced professional efficacy. Burnout literally drains your cognitive and emotional energy, leaving you physically weak and apathetic.
9. Lifestyle and Environmental Factors

Sometimes, the culprit behind feeling weak after resting is embedded in our daily habits and environments.
Dehydration
Water is essential for every cellular process, including ATP production. Even mild dehydration (as little as 1-2% of body weight) can cause a significant drop in energy levels, impair cognitive function, and lead to muscle weakness. Since we lose water through respiration and sweat while we sleep, waking up dehydrated is a common cause of morning lethargy.
Sedentary Lifestyle
It seems counterintuitive, but resting too much can make you feel weak. The human body operates on a “use it or lose it” principle. A highly sedentary lifestyle leads to muscle deconditioning and decreased cardiovascular efficiency. When you lack physical fitness, even basic daily tasks require a higher percentage of your maximum effort, making you feel weak and easily fatigued.
Over-Reliance on Caffeine and Alcohol
While caffeine blocks adenosine receptors (the chemical that makes you feel sleepy), it does not actually give you energy; it just borrows it from the future. A severe caffeine crash can make your limbs feel heavy and weak.
Alcohol, on the other hand, is a severe sleep disruptor. While a drink might help you fall asleep faster, it destroys your sleep architecture, suppressing REM sleep and causing micro-awakenings throughout the second half of the night.
10. When to See a Doctor: The Diagnostic Workup
If you have optimized your sleep hygiene, diet, and lifestyle, and you still wake up feeling profoundly weak, it is time to seek medical intervention. Chronic weakness is a symptom, not a disease in itself.
Be an advocate for your health. When you visit your doctor, clearly articulate the difference between being “sleepy” and feeling “physically weak.”
Table 3: Suggested Blood Tests for Unexplained Weakness
| Test Panel | What it Checks | Why it Matters |
| Complete Blood Count (CBC) | Red/White blood cells, hemoglobin. | Checks for various types of anemia and active infections. |
| Comprehensive Metabolic Panel (CMP) | Kidney/liver function, electrolytes, glucose. | Identifies blood sugar issues, electrolyte imbalances, or organ dysfunction. |
| Full Thyroid Panel | TSH, Free T3, Free T4, Thyroid Antibodies. | Identifies hypothyroidism or autoimmune thyroid conditions (Hashimoto’s). |
| Iron Panel & Ferritin | Serum iron, transferrin, ferritin. | Ferritin measures stored iron; standard tests often miss low iron stores. |
| Vitamin Levels | Vitamin D (25-OH), Vitamin B12, Folate. | Detects common deficiencies that cause muscle weakness and neurological fatigue. |
| C-Reactive Protein (CRP) / ESR | Systemic inflammation markers. | Elevated levels indicate ongoing inflammation, auto-immune issues, or infection. |
11. Actionable Strategies for True Restoration
Understanding the root causes of your weakness is the first step. The next is implementing changes to heal your body and restore your energy.
1. Optimize Your Sleep Environment
Treat your bedroom as a sanctuary for sleep.
- Temperature: Keep the room cool (around 65°F or 18°C). A drop in core body temperature is required to initiate deep sleep.
- Light: Use blackout curtains. Even a small amount of ambient light can disrupt melatonin production. Expose your eyes to bright, natural sunlight within 30 minutes of waking up to set your circadian rhythm.
- Digital Curfew: Stop looking at screens (phones, TVs, tablets) at least an hour before bed. Blue light suppresses melatonin.
2. Hydrate Before You Caffeinate
Before pouring your morning coffee, drink a large glass of water, ideally with a small pinch of high-quality sea salt to replenish electrolytes lost overnight. Rehydrating your cells immediately boosts blood volume and energy.
3. Eat for Sustained Energy
Avoid starting your day with pure carbohydrates or sugars (like pastries or sugary cereals). This sets off a blood sugar roller coaster. Instead, focus on a breakfast rich in high-quality protein, healthy fats, and complex carbohydrates (e.g., eggs, avocados, and oatmeal) to provide a slow, steady release of energy.
4. Engage in Graded Movement
If you are deconditioned, do not start with high-intensity interval training. Begin with gentle movement like walking, yoga, or stretching. Movement increases blood flow, delivers oxygen to your tissues, and stimulates the creation of new mitochondria in your cells (mitochondrial biogenesis). Note: If you suspect you have ME/CFS, consult a specialist before increasing exercise, as it can trigger severe post-exertional malaise.
5. Manage the Cognitive Load
If anxiety or depression is draining your energy, recognize that mental health care is physical health care. Practices like mindfulness, cognitive-behavioral therapy (CBT), or journaling can help lower your baseline cortisol levels, taking your nervous system out of “fight or flight” mode and allowing your body to actually rest when you lie down.
Conclusion
Feeling weak even after rest is a complex, multi-layered issue that extends far beyond simply needing more hours in bed. It is a biological distress signal indicating a disruption in your sleep architecture, cellular energy production, nutritional status, hormonal balance, or mental well-being.
Validating your experience is the most important first step: you are not lazy, and your exhaustion is real. By systematically investigating the potential culprits—from sleep apnea and iron deficiency to thyroid dysfunction and chronic stress—and working in partnership with healthcare professionals, you can uncover the specific reasons behind your weakness. With patience, targeted interventions, and deep systemic care, it is possible to repair your body’s energy pathways and wake up feeling genuinely restored, capable, and strong.
Scientific References and Further Reading
- Walker, M. (2017). Why We Sleep: Unlocking the Power of Sleep and Dreams. Scribner. (A comprehensive review of sleep architecture and the physiological consequences of sleep deprivation).
- Institute of Medicine (US) Committee on Sleep Medicine and Research. (2006). Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington (DC): National Academies Press (US).
- López-Lluch, G., et al. (2016). “Mitochondrial biogenesis and healthy aging.” Experimental Gerontology, 81, 10-15. (Explores the role of mitochondria in cellular energy and systemic fatigue).
- Zimmermann, M. B., & Hurrell, R. F. (2007). “Nutritional iron deficiency.” The Lancet, 370(9586), 511-520. (Detailed clinical data on how iron deficiency impacts oxygen transport and energy).
- Holick, M. F. (2007). “Vitamin D deficiency.” The New England Journal of Medicine, 357(3), 266-281. (A definitive review of Vitamin D’s role in skeletal muscle weakness and general health).
Chrousos, G. P. (2009). “Stress and disorders of the stress system.” Nature Reviews Endocrinology, 5(7), 374-381. (An analysis of HPA axis dysregulation, cortisol levels, and chronic stress-induced fatigue).
Emily Carter is a Senior Health Researcher and Supplement Analyst at the Nutrasfit Research Team, based in Austin, Texas. She specializes in evaluating dietary supplements through ingredient analysis, scientific research, and real-world effectiveness.
With a background in nutrition science, Emily focuses on breaking down complex health information into simple, practical insights that readers can trust. Her work is centered on helping individuals make informed decisions and choose supplements that are safe, effective, and aligned with their health goals.