
The human gastrointestinal (GI) tract is often referred to as the body’s “second brain.” Trillions of bacteria, viruses, and fungi coexist within our digestive system, collectively known as the gut microbiome. According to theHarvard T.H. Chan School of Public Health, these microorganisms play a vital role in our overall health, influencing everything from nutrient absorption and immune system function to mood regulation and chronic disease prevention.
When your gut microbiome is balanced, digestion is smooth, and systemic inflammation is kept at bay. However, modern lifestyles are rife with habits and dietary choices that disrupt this delicate ecosystem, leading to a state called dysbiosis—an imbalance of gut microbial communities. This can result in bloating, gas, indigestion, fatigue, and even long-term conditions like Irritable Bowel Syndrome (IBS) or Inflammatory Bowel Disease (IBD) (Wikipedia: Dysbiosis).
To optimize your digestive health, it is equally important to know what not to do as it is to know what to eat. This deep, informational guide breaks down the science behind 10 things you must avoid for better digestion and gut health, backed by scientific literature and trusted health resources.
The Foundation of Gut Health
Before diving into what to avoid, it is crucial to understand how the gut functions. Digestion is not just a mechanical process; it is highly chemical and microbiological. The Enteric Nervous System (ENS) governs the function of the gastrointestinal tract and communicates directly with the brain via the vagus nerve—a connection known as the gut-brain axis.
Table 1: Key Components of the Gut Microbiome
| Bacterial Phyla / Component | Primary Function within the Human Gut | Health Implication if Imbalanced |
| Bacteroidetes | Breaks down complex carbohydrates and produces beneficial short-chain fatty acids (SCFAs). | Low levels are associated with obesity, inflammation, and metabolic syndrome. |
| Firmicutes | Plays a role in energy absorption and metabolism. | A high Firmicutes-to-Bacteroidetes ratio is strongly linked to obesity. |
| Actinobacteria | Contains Bifidobacteria, crucial for breaking down dietary fiber and preventing infection. | Depletion can lead to weakened immune responses and poor digestion. |
| Proteobacteria | Normally present in small amounts; includes pathogens like E. coli and Salmonella. | Overgrowth indicates severe dysbiosis and high systemic inflammation. |
| Mucin Layer | A protective mucous barrier lining the intestinal wall. | Degradation leads to “leaky gut,” allowing toxins into the bloodstream. |
(Source integration adapted from National Institutes of Health (NIH) – Gut Microbiome in Health and Disease)
1. Ultra-Processed Foods and Chemical Emulsifiers
The Problem
Ultra-processed foods (UPFs) are formulations of ingredients derived from foods and additives. Think of packaged baked goods, instant noodles, sugary cereals, and industrially manufactured snacks. These foods are explicitly engineered for hyper-palatability and long shelf lives, but they spell disaster for your gut.
The Scientific Mechanism
The danger of UPFs lies not just in their lack of nutrients, but in their chemical additives, particularly emulsifiers. Emulsifiers like carboxymethylcellulose (CMC) and polysorbate-80 (P80) are added to foods to improve texture and prevent separation (e.g., keeping oil and water mixed in salad dressings).
A landmark study published in the journal Nature demonstrated that dietary emulsifiers directly alter the gut microbiota, promoting inflammation. These chemicals act almost like detergents in the gut, breaking down the crucial mucous layer that lines the intestinal wall (refer to Table 1). When this mucosal barrier is compromised, gut bacteria come into direct contact with the intestinal cells, triggering an inflammatory immune response and leading to increased intestinal permeability, commonly known as Leaky Gut Syndrome (Nature: Dietary emulsifiers impact the mouse gut microbiota).
Furthermore, ultra-processed foods are typically devoid of dietary fiber, starving the beneficial bacteria in your lower intestine that rely on complex carbohydrates to survive.
What to Do Instead
- Embrace Whole Foods: Shift your diet towards foods in their natural state—vegetables, fruits, whole grains, lean proteins, and healthy fats.
- Read Labels: Avoid products with long, unpronounceable ingredient lists. Specifically look out for “polysorbate,” “carboxymethylcellulose,” “carrageenan,” and “guar gum” if you have a sensitive stomach.
- Cook at Home: Preparing your meals is the only foolproof way to control exactly what enters your digestive tract.
2. Diets High in Added Sugars and Refined Carbohydrates
The Problem
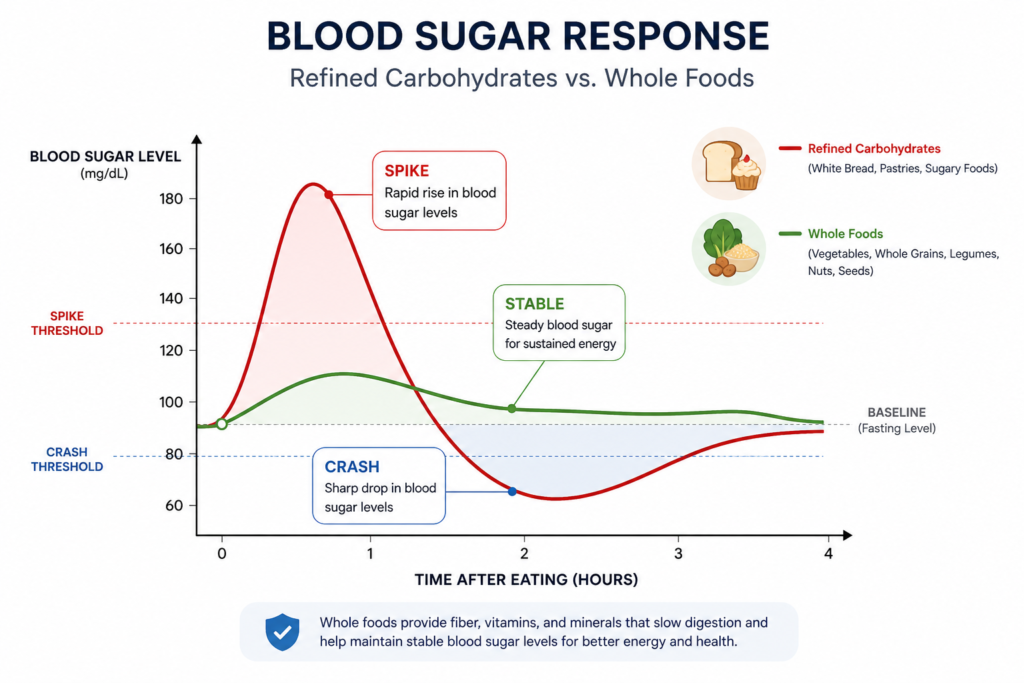
The modern Western diet is heavily reliant on added sugars (like high-fructose corn syrup) and refined carbohydrates (like white bread, white pasta, and pastries). While these foods provide immediate energy, they bypass the lower gut and cause rapid spikes in blood sugar, wreaking havoc on the digestive system.
The Scientific Mechanism
Added sugars and simple carbohydrates are absorbed very quickly in the small intestine. This rapid absorption leaves virtually nothing for the beneficial microbes in the large intestine to feed on. Worse, diets high in refined sugar actively feed pathogenic and opportunistic microbes, such as the yeast Candida albicans and harmful strains of Clostridium.
Research published by the American Society for Microbiology highlights that high-sugar diets drastically reduce microbial diversity. Furthermore, excessive sugar intake promotes the production of advanced glycation end products (AGEs) and pro-inflammatory cytokines, which irritate the intestinal lining.
Fructose, in particular, when consumed in massive quantities (like in sodas), can lead to fructose malabsorption. The unabsorbed fructose ferments in the colon, drawing in water and producing gas, which leads to bloating, cramping, and osmotic diarrhea (Mayo Clinic: Fructose Intolerance).
What to Do Instead
- Opt for Complex Carbs: Replace white rice, white bread, and traditional pasta with quinoa, brown rice, oats, and whole-wheat alternatives.
- Satisfy Sweet Cravings Naturally: Use whole fruits, which contain natural sugars bound with dietary fiber. The fiber slows down sugar absorption and feeds beneficial bacteria.
- Monitor Hidden Sugars: Check nutrition labels on savory items like pasta sauces, condiments, and salad dressings, which are notorious for hiding high-fructose corn syrup.
3. Unnecessary Use of Antibiotics
The Problem
Antibiotics are one of the greatest achievements of modern medicine, saving millions of lives from bacterial infections. However, their overuse—and use for viral infections where they are ineffective—is a leading cause of long-term digestive distress.
The Scientific Mechanism
Antibiotics are generally non-selective. Broad-spectrum antibiotics operate like a biological “scorched earth” campaign; they wipe out the pathogenic bacteria causing an illness, but they simultaneously eradicate vast populations of beneficial microbes in the gut.
This mass extinction event within the gut microbiome causes immediate acute symptoms like antibiotic-associated diarrhea. Long-term, it leads to severe dysbiosis. Without the protective presence of beneficial bacteria, opportunistic and dangerous pathogens like Clostridioides difficile (C. diff) can multiply rapidly, causing severe, life-threatening colon inflammation (Wikipedia: Clostridioides difficile infection).
Studies show that even a single course of broad-spectrum antibiotics can alter the microbiome for months, and in some individuals, certain bacterial strains may never fully recover without deliberate dietary and supplemental interventions (PubMed: Impacts of antibiotics on the human microbiome).
What to Do Instead
- Question Prescriptions: Only take antibiotics when prescribed by a doctor for a confirmed bacterial infection. Do not pressure physicians for antibiotics when suffering from viral infections like the common cold or flu.
- Support with Probiotics: If you must take antibiotics, consider supplementing with clinically studied probiotics (like Saccharomyces boulardii or Lactobacillus rhamnosus GG) two hours apart from your antibiotic dose.
- Eat Fermented Foods: Incorporate kefir, sauerkraut, kimchi, and plain yogurt into your diet to help reintroduce beneficial microbes post-treatment.
4. Excessive Alcohol Consumption
The Problem
While an occasional glass of red wine is often touted for its polyphenol content, excessive or binge drinking is highly toxic to the gastrointestinal system. The gut is the first point of contact for alcohol, and heavy consumption compromises every stage of digestion.
The Scientific Mechanism
When you consume alcohol, a portion is absorbed directly through the stomach lining, but the majority enters the small intestine. High concentrations of alcohol act as a solvent, damaging the mucosal lining of the stomach and intestines. This irritation can lead to gastritis (inflammation of the stomach lining) and acid reflux.
More critically, alcohol is metabolized into acetaldehyde, a toxic compound. Alcohol and its metabolites impair the tight junction proteins that hold intestinal cells together. This creates massive intestinal permeability (leaky gut). Once the barrier is broken, bacterial toxins called lipopolysaccharides (LPS) escape the gut and enter the bloodstream. This triggers a massive systemic inflammatory response and forces the liver to work overtime, linking gut damage directly to liver disease (the gut-liver axis) (National Institute on Alcohol Abuse and Alcoholism (NIAAA)).
Furthermore, chronic alcohol consumption drastically alters the microbiome, promoting the overgrowth of Proteobacteria (often pathogenic) while depleting anti-inflammatory Firmicutes and Bacteroidetes.
What to Do Instead
- Practice Moderation: If you choose to drink, adhere to established guidelines: up to one drink per day for women and two for men.
- Hydrate Continuously: Drink a glass of water for every alcoholic beverage to dilute the alcohol concentration in your GI tract.
- Focus on Polyphenols: If seeking the heart and gut benefits of red wine, you can obtain the exact same polyphenols (like resveratrol) from eating red grapes, berries, and dark chocolate without the toxic effects of ethanol.
5. Chronic Stress and Anxiety
The Problem
Digestion is not purely a physical process; it is deeply psychological. Have you ever felt “butterflies” in your stomach when nervous, or lost your appetite during a stressful event? That is the gut-brain axis at work. Chronic, unmanaged stress is one of the most potent destroyers of gut health.
The Scientific Mechanism
The autonomic nervous system has two main modes: the sympathetic (“fight or flight”) and the parasympathetic (“rest and digest”).
When you experience chronic stress, your brain constantly signals the adrenal glands to release cortisol and adrenaline. The body prioritizes survival over digestion. Blood flow is diverted away from the gastrointestinal tract and toward the muscles and brain. Digestive enzyme production halts, stomach acid secretion drops, and gut motility (the muscular contractions that move food through the intestines) slows down or spasms.
This state leads to malabsorption of nutrients, severe bloating, and constipation or diarrhea. Furthermore, chronic stress actually alters the composition of the microbiome. High cortisol levels decrease the production of Secretory IgA (sIgA), an antibody that protects the mucosal lining, making the gut vulnerable to pathogens and increasing intestinal permeability (Harvard Health: The gut-brain connection).
Table 2: The Gut-Brain Axis: How Stress Manifests Physically
| Stress Response / Mechanism | Effect on Gastrointestinal Tract | Common Symptoms Experienced |
| Increased Cortisol Release | Suppresses immune function in the gut; thins mucosal lining. | Increased food sensitivities, leaky gut, inflammation. |
| Vagus Nerve Suppression | Inhibits the “rest and digest” parasympathetic state. | Low stomach acid, delayed gastric emptying, indigestion. |
| Altered Gut Motility | Muscle contractions become erratic (too fast or too slow). | Diarrhea (if too fast), Constipation (if too slow), abdominal cramps. |
| Decreased Blood Flow | Reduced oxygen and nutrients delivered to digestive organs. | Poor nutrient absorption, fatigue after eating. |
What to Do Instead
- Mindful Eating: Take 5 deep breaths before every meal to activate the vagus nerve and manually shift your body into a parasympathetic state.
- Stress Management: Incorporate daily practices like meditation, yoga, or simple nature walks to lower baseline systemic cortisol.
- Chew Thoroughly: Chewing is a rhythmic action that naturally signals to the brain that you are safe, helping to lower stress responses during meals.
6. Non-Nutritive Artificial Sweeteners
The Problem
In an attempt to avoid the harms of sugar, millions of people turn to zero-calorie artificial sweeteners found in diet sodas, sugar-free snacks, and protein powders. While they may save calories, emerging evidence suggests they exact a heavy toll on the gut microbiome.
The Scientific Mechanism
Artificial sweeteners like sucralose (Splenda), saccharin (Sweet’N Low), and aspartame (Equal) pass through the human digestive system without being broken down for energy. However, they do not pass through unnoticed by our gut bacteria.
A groundbreaking study by the Weizmann Institute of Science revealed that non-nutritive sweeteners drastically alter the composition of the gut microbiota. The researchers found that consuming these sweeteners led to an overgrowth of bacteria that are highly efficient at extracting energy from food, ironically leading to glucose intolerance and an increased risk of metabolic syndrome—the very conditions diet products are marketed to prevent.
Furthermore, studies have indicated that sucralose can decrease beneficial Lactobacillus and Bifidobacterium species in the gut by up to 50% in animal models, while simultaneously increasing the gut’s pH, creating an environment where pathogenic bacteria can thrive.
What to Do Instead
- Natural Alternatives: Opt for natural, minimally processed sweeteners like small amounts of raw honey or pure maple syrup, which have antibacterial and antioxidant properties.
- Stevia and Monk Fruit: If a zero-calorie option is necessary, natural extracts like high-quality Stevia or Monk Fruit (without added sugar alcohols like erythritol) appear to be gentler on the gut, though they should still be consumed in moderation.
- Acclimate Your Palate: Gradually reduce the sweetness of your foods and beverages. Over time, your taste buds will adapt, and you won’t crave intensely sweet flavors.
7. Poor Sleep Hygiene and Sleep Deprivation
The Problem
You might not associate your sleep habits with your digestion, but the two are intimately linked. Poor sleep hygiene, erratic sleep schedules, and chronic sleep deprivation profoundly disrupt the microbial rhythms in your gut.
The Scientific Mechanism
Just as humans have a circadian rhythm (a 24-hour internal clock dictating sleep-wake cycles), the gut microbiome has its own circadian rhythm. Different strains of bacteria fluctuate in abundance and activity depending on the time of day.
When you experience sleep deprivation, or if you work night shifts and experience “circadian misalignment,” it directly alters the gut flora. A study published in the journal Molecular Metabolism showed that just two nights of partial sleep deprivation resulted in a significant shift in the microbiome, specifically an increase in the Firmicutes-to-Bacteroidetes ratio—a microbial profile closely associated with metabolic disruption and obesity (PubMed: Gut microbiome and sleep).
Furthermore, poor sleep increases systemic stress (cortisol), which, as discussed earlier, degrades the gut lining. Lack of sleep also disrupts the hormones ghrelin (the hunger hormone) and leptin (the satiety hormone), leading to cravings for ultra-processed, sugary foods that further damage the gut.
What to Do Instead
- Consistent Sleep Schedule: Go to bed and wake up at the exact same time every day, even on weekends, to stabilize both your bodily and microbial circadian rhythms.
- Fasting Before Bed: Stop eating at least 3 hours before sleep. This gives your digestive system time to process food and run its “cleaning cycle” (the migrating motor complex) overnight.
- Optimize Your Environment: Ensure your bedroom is cool, completely dark, and free of blue light-emitting electronics at least an hour before bed.
8. Smoking and Tobacco Use
The Problem
It is universally understood that smoking causes lung cancer and cardiovascular disease. However, its devastating effects on the gastrointestinal tract and the gut microbiome are often overlooked. Smoking drastically increases the risk of serious digestive disorders.
The Scientific Mechanism
Cigarette smoke contains over 4,000 chemicals, dozens of which are known carcinogens. When smoke is inhaled, these toxins enter the bloodstream and systematically affect every organ, including the digestive tract.
Smoking relaxes the lower esophageal sphincter, the valve between the esophagus and the stomach, leading to severe acid reflux and Gastroesophageal Reflux Disease (GERD). Furthermore, smoking decreases blood flow to the gut lining, impairing its ability to heal and regenerate, making smokers highly susceptible to peptic ulcers (WebMD: Smoking and the Digestive System).
Crucially, smoking completely alters the gut microbiome. Studies show that smokers have significantly higher levels of Clostridium and Bacteroides and lower levels of beneficial Bifidobacteria. This dysbiosis is so severe that smoking is identified as one of the most significant environmental risk factors for developing Crohn’s disease, a debilitating form of Inflammatory Bowel Disease (IBD) (Wikipedia: Crohn’s disease).
What to Do Instead
- Quit Smoking entirely: There is no safe level of tobacco use for gut health. Seek out smoking cessation programs, nicotine replacement therapies, or behavioral counseling.
- Avoid Secondhand Smoke: The systemic inflammatory effects of smoke can be triggered even if you are not the primary smoker.
- Post-Quitting Gut Rehab: When quitting, actively support your gut with high-fiber foods and prebiotics, as the microbiome goes through a transitional phase of healing.
9. Eating Too Quickly and Poor Mastication
The Problem
In our fast-paced society, meals are often eaten in a rush—wolfed down at a desk, in a car, or while distracted by a smartphone. Eating too quickly and failing to chew food properly is a primary trigger for indigestion, bloating, and gas.
The Scientific Mechanism
Digestion does not begin in the stomach; it begins in the brain and the mouth. The “cephalic phase” of digestion occurs when you see, smell, and anticipate food, triggering the release of saliva and gastric juices. If you eat mindlessly, you bypass this crucial preparatory phase.
Once food is in the mouth, mastication (chewing) serves a mechanical and chemical purpose. Mechanically, breaking food into smaller pieces increases the surface area for stomach acid and enzymes to act upon. Chemically, saliva contains an enzyme called salivary amylase, which begins the breakdown of complex carbohydrates immediately.
If food is swallowed whole, the stomach has to work incredibly hard to break it down. Large, undigested food particles pass into the small intestine, where they cannot be properly absorbed. They eventually reach the large intestine, where bacteria ferment these large particles, producing massive amounts of gas, leading to severe bloating and flatulence. Furthermore, eating fast prevents the hormone cholecystokinin (CCK) from signaling fullness to the brain in time, leading to overeating and excessive pressure on the GI tract.
What to Do Instead
- The 20-Chew Rule: Aim to chew each bite of food 15 to 20 times, or until it reaches a liquid consistency, before swallowing.
- Put Your Fork Down: Actively put your utensils down between bites to force a slower pace.
- Eliminate Distractions: Do not eat while watching TV or working. Focus on the sensory experience of the food to optimize the cephalic phase of digestion.
10. A Sedentary Lifestyle
The Problem
A lack of physical activity is detrimental to nearly every system in the human body, and the digestive system is no exception. Sitting for prolonged periods slows down bodily functions, leading to sluggish digestion and a stagnating microbiome.
The Scientific Mechanism
Physical activity directly stimulates peristalsis—the series of wave-like muscle contractions that move food through the digestive tract. When you are sedentary, gut motility slows down dramatically. This increases transit time (the time it takes for food to pass from mouth to anus). Prolonged transit time means that water is excessively absorbed from the stool in the colon, leading to hard, difficult-to-pass stools and chronic constipation.
Fascinatingly, exercise independent of diet has been shown to alter the gut microbiome. A study investigating the microbiomes of professional athletes (such as rugby players) found that they possessed significantly higher microbial diversity and higher levels of Akkermansia muciniphila, a bacterium associated with a healthy metabolic profile and lower systemic inflammation, compared to sedentary individuals (NIH PubMed: Exercise and Gut Microbiome).
Exercise also reduces systemic inflammation and helps manage cortisol levels, both of which indirectly support a healthy intestinal barrier.
What to Do Instead
- Daily Movement: Aim for at least 30 minutes of moderate-intensity exercise, such as brisk walking, cycling, or swimming, most days of the week.
- Post-Meal Walks: Taking a gentle 10-to-15-minute walk immediately after meals has been scientifically proven to accelerate gastric emptying, reduce bloating, and regulate blood sugar spikes.
- Break Up Sitting: If you work a desk job, set a timer to stand up, stretch, or do a few twists every hour to stimulate blood flow to the digestive organs.
Table 3: Actionable Swaps for Better Gut Health
| Gut-Damaging Habit / Food | Healthier, Gut-Friendly Alternative | Primary Benefit to the Digestive System |
| Drinking Diet Soda (Sucralose/Aspartame) | Sparkling water with a squeeze of fresh lemon or lime. | Avoids chemical disruption of the microbiome; provides hydration. |
| Eating highly processed white bread | Sourdough bread or 100% whole grain bread. | Sourdough fermentation pre-digests gluten and provides good bacteria. |
| Managing stress with alcohol | Yoga, deep breathing exercises, or a warm bath. | Prevents leaky gut; activates the parasympathetic (rest/digest) system. |
| Swallowing food after 2-3 chews | Chewing each bite until it is a paste (15-20 times). | Enhances salivary amylase action; prevents fermentation gas in the colon. |
| Sitting immediately after a heavy meal | Taking a 15-minute gentle stroll outside. | Mechanically stimulates peristalsis and aids stomach emptying. |
Conclusion
Optimal digestion and gut health are not achieved purely through taking expensive probiotic supplements. True gut health requires a holistic approach, focused heavily on the removal of damaging irritants and behaviors. The gut microbiome is incredibly resilient, but it requires a hospitable environment to thrive.
By actively avoiding ultra-processed foods, artificial sweeteners, chronic stress, and a sedentary lifestyle, you stop the continuous assault on your intestinal lining. When you pair this avoidance with positive habits—such as eating high-fiber whole foods, practicing mindful eating, prioritizing sleep, and engaging in regular physical activity—you allow your digestive system to heal. Over time, cultivating these habits will foster a robust, diverse microbiome, leading to smoother digestion, enhanced immunity, and a profound improvement in your overall vitality and well-being.
References and Further Reading
- Harvard T.H. Chan School of Public Health: The Microbiome. Comprehensive overview of how gut bacteria influence human health. Available at Harvard Nutrition Source.
- Nature Journal: Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Chassaing B, et al. (2015). Demonstrates the destructive nature of common food additives on the intestinal mucus layer.
- National Institutes of Health (NIH): Gut Microbiome in Health and Disease. A deep dive into bacterial phyla and their systemic effects. Available on PMC.
- Weizmann Institute of Science: Artificial sweeteners and the microbiome. Elinav, E., et al. (2014). Research outlining how non-nutritive sweeteners induce glucose intolerance. Read the summary here.
- Harvard Health Publishing: The gut-brain connection. Explains the enteric nervous system and how psychological stress translates to physical digestive symptoms. Available at Harvard Health.
- Mayo Clinic: Fructose Intolerance and Digestive Distress. Guidelines on identifying and managing the malabsorption of dietary sugars. Available at Mayo Clinic.
- Wikipedia Resources for Foundational Concepts:
- Enteric Nervous System
- Dysbiosis
- Short-chain fatty acids
- National Institute on Alcohol Abuse and Alcoholism (NIAAA): Outlines the pathological effects of alcohol on the gut-liver axis and mucosal integrity. NIAAA Official Site.
- American Society for Microbiology: The Impact of Diet on Gut Microbiota. Reviews the detrimental effects of refined carbohydrates versus complex dietary fibers.
Emily Carter is a Senior Health Researcher and Supplement Analyst at the Nutrasfit Research Team, based in Austin, Texas. She specializes in evaluating dietary supplements through ingredient analysis, scientific research, and real-world effectiveness.
With a background in nutrition science, Emily focuses on breaking down complex health information into simple, practical insights that readers can trust. Her work is centered on helping individuals make informed decisions and choose supplements that are safe, effective, and aligned with their health goals.